Winter slips happen fast. One second you’re walking, the next you’re on the ground wondering what just happened.
Ice related falls are one of the most common causes of injury during winter, and they don’t just affect older adults. We regularly see active adults, workers, runners, and parents injured after a simple slip on icy sidewalks, driveways, or parking lots.
The tricky part? These injuries don’t always feel serious right away. Pain can show up days later or quietly linger until it starts interfering with daily life.
Why Ice Related Falls Cause These Injuries
When you slip on ice, your body reacts instinctively. You try to catch yourself, twist away, or brace for impact, often all at once.
That sudden, uncontrolled movement puts stress on areas that aren’t prepared to absorb force, especially the hips, wrists, and shoulders.
Unlike sports injuries where the body may be warmed up and moving predictably, winter falls usually happen:
- Without warning
- With poor footing
- In awkward positions
This combination increases the risk of strain, joint irritation, and even fractures.
Hip Injuries After a Fall
The hips take a lot of force during a slip, especially if you land sideways or twist as you fall.
Common hip related issues we see include:
- Deep hip or groin pain
- Bruising and stiffness
- Difficulty walking or climbing stairs
- Pain that worsens after sitting or standing too long
Sometimes the pain isn’t directly in the hip joint itself. Muscles, tendons, or surrounding structures may be overloaded, leading to lingering discomfort if not addressed properly
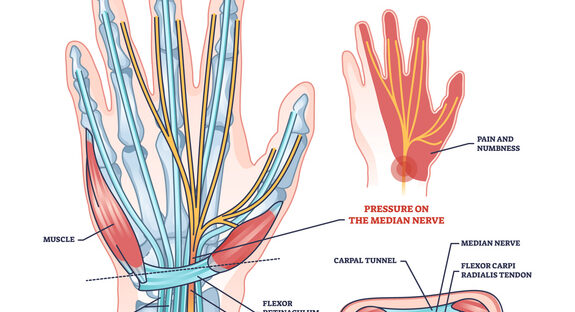
Wrist Injuries: The Natural “Catch”
Most people instinctively put their hands out to break a fall. Unfortunately, the wrist isn’t designed to absorb your full body weight suddenly.
Common wrist injuries after ice-related falls include:
- Wrist sprains or strains
- Ligament irritation
- Tendon inflammation
- Fractures (especially with more forceful falls)
Even if X-rays show no fracture, wrist pain can persist if swelling, stiffness, or loss of strength isn’t properly managed.
Shoulder Injuries From Bracing or Impact
Shoulder injuries often happen when someone lands on an outstretched arm or shoulder.
Symptoms can include:
- Pain when lifting the arm
- Night pain when lying on the affected side
- Weakness or instability
- Limited range of motion
Because the shoulder relies heavily on muscle coordination, even a minor fall can disrupt how the joint moves, leading to pain that sticks around longer than expected.
Why These Injuries Can Linger
One of the biggest frustrations after a winter fall is that pain doesn’t always improve on its own.
Common reasons symptoms linger include:
- Loss of strength after injury
- Joint stiffness and reduced mobility
- Altered movement patterns to “protect” the area
- Returning to activity too quickly
Pain may settle initially, but without restoring strength, control, and tolerance, the injury often resurfaces during normal daily activities.
How Physiotherapy Helps After a Winter Fall
Physiotherapy focuses on more than just pain relief.
Treatment after an ice-related fall often includes:
- Assessing how the joint and surrounding muscles are moving
- Restoring strength and mobility safely
- Improving balance and coordination
- Gradually reintroducing daily and work activities
- Preventing future falls and repeat injuries
Addressing the injury early helps reduce the risk of chronic pain and recurring flare-ups.
When to Seek Physiotherapy After a Fall
You should consider physiotherapy if:
- Pain hasn’t improved after a few days
- You notice stiffness, weakness, or limited movement
- Daily tasks feel harder than before
- Pain returns when you try to be active again
Ignoring these signs can lead to longer recovery times and unnecessary setbacks.
Ice related falls may seem minor at first, but hip, wrist, and shoulder injuries can quietly turn into long-term issues if left untreated.
Early assessment, proper movement, and gradual strengthening can make the difference between a quick recovery and months of frustration.
If you’ve had a fall this winter and something doesn’t feel right, contact the team at Durham Orthopedic & Sports Injury Clinic to help assess the injury and guide you back to confident, pain free movement.